Vitiligo Treatment
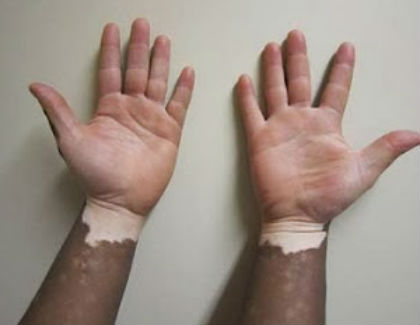
Vitiligo is a disorder in which depigmented(white) patches of skin appear on different parts of the body.In vitiligo the pigment cells of the skin, melanocytes, are destroyed.Vitiligo can be focal and localized to one area, or it may affect several different areas on the body. Vitiligo can also affect the mucous membranes (such as the tissue inside the mouth and nose) or the genitals.
The exact cause of vitiligo is unknown, although it is believed that it is an autoimmune condition in which the body’s immune system mistakenly attacks and destroys certain cells within the body.
What causes vitiligo?
The cause is not known. Vitiligo may be an autoimmune disease. These diseases happen when your immune system mistakenly attacks some part of your own body. In vitiligo, the immune system may destroy the melanocytes in the skin. It is also possible that one or more genes may make a person more likely to get the disorder.
There is no way to tell if vitiligo will spread, its prognosis is unpredictable. For some people, the white patches do not spread. But often the white patches will spread to other areas of the body. For some people, vitiligo spreads slowly, over many years. For other people, spreading occurs quickly. Some people have reported more white patches after physical or emotional stress.
How is vitiligo diagnosed?
The doctor will use a family and medical history, physical examination and few clinical tests to diagnose vitiligo.
Can my kids develop these patches?
Vitiligo does have a genetic transmissible potential. However risk is higher if the disease is present in more than one generation or if both parents have vitiligo.
Is this contagious?
No, vitiligo is not contagious and does not spread even from close contact.
Is it Treatable?
Yes, you need to be patient. Treatments may at times be neede for a longer period of time. Results are best obtained when the disease is limited to few patches and treatment is sought early.
Treatment Options
Current treatment options for vitiligo include medical, surgical, and Phototherapy. Most treatments are aimed at restoring color of the white patches of skin.
The choice of treatment depends on:
- The number of white patches
- Disease stability
- The personal patient profile like age, social circumstances etc.
Same treatment is not right for everyone. Many treatments can have unwanted side effects. Treatments can take a long time, and sometimes they don’t work.
Medical treatments
Topical preparations:
- A topical steroid preparation is often chosen first to treat localized vitiligo. The results of therapy have been reported as moderately successful, particularly in patients with localized vitiligo.
- Topical calcineurin inhibitors (such as tacrolimus or pimecrolimus) (0.03% or 0.1%) are an effective alternative therapy for vitiligo, particularly when the disease involves the head and neck.
- Vitamin D analogs, particularly calcipotriol and tacalcitol, have also been used. They target the local immune response and act on specific T-cell activation.
Systemic therapy
- Steroids have been reported anecdotally to achieve success when given in pulse doses or low doses to minimize its adverse effects. The benefits versus the toxicity of this therapy must be weighed carefully. More research is necessary to establish the safety and effectiveness of this therapy for vitiligo.
- Psoralenes : these are photo active agents that help in growth of melanocytes. They are usually give along with photo-therapy.
- Topical PUVA is of benefit in some patients with localized lesions. Cream and solution of 8-methoxypsoralen (0.1-0.3% concentration) are available for this treatment. It is applied 30 minutes prior to UV-A radiation (usually 0.1-0.3 J/cm2 UV-A) exposure. It should be applied once or twice a week
Phototherapy
Phototherapy is considered to be a second-line treatment for vitiligo. It involves exposing the white patches to high but controlled doses of Ultraviolet radiations. This can be done in form of UVA or UVB.
Exposing the skin to UVB light from UVB lamps is the most common treatment for vitiligo. The treatments can be done at home with a domestic UVB lamp or in a clinic. It is important to control the exposure time so that the skin does not burn from overexposure. Treatment can take a few to more than 3 years,varying from patient to patient. Phototherapy sessions are done 2–3 times a week. Spots on a large area of the body may require full body treatment in a clinic or hospital. Narrowband UVB with a wavelength of 311 nm is the phototherapy of choice. Narrowband ultraviolet B (NBUVB) phototherapy lacks the side-effects caused by psoralens. This treatment can be safely used in children, pregnant women, and lactating women. Short-term adverse effects include pruritus, tanning and xerosis. It has been constitutively reported that combination of UVB phototherapy with other topical treatments improves repigmentation.
Ultraviolet light (UVA) treatments are normally carried out in clinics. Psoralen and ultraviolet A light (PUVA) treatment involves taking a drug that increases the skin’s sensitivity to ultraviolet light, then exposing the skin to high doses of UVA light. Treatment is required twice a week for 6–12 months or longer. Because of the high doses of UVA and psoralen, PUVA may cause side effects such as sunburn-type reactions or skin freckling.
Surgical Treatments
This is best suited for patients who have
- No progression of lesions for at least 1 year.
- Absence of new koebnerization, indicating disease inactivity.
- Unilateral vitiligo most stable form of vitiligo.
- Limited nos of patches on exposed sites not responding to other therapies.
Five basic methods for repigmentation surgery
- Thin dermoepidermal graft/ Split thickness Graftings: The depigmented skin (epidermis) is removed by superficial dermabrasion, including the papillary dermis, and very thin dermoepidermal sheets harvested from patients own thigh or arm is placed on the patch.
- Noncultured epidermal suspensions: After the achromic epidermis is removed, an epidermal suspension with melanocytes and keratinocytes previously prepared by trypsinization of normally pigmented donor skin is spread onto the denuded area and immediately covered with nonadherent dressings. Using noncultured epidermal cellular grafts
- Suction epidermal graftingThis is best suited for areas like Lips, face or nipples around breast. Artificial blisters are prepared on donor areas and roof of these blisters are transplanted onto dermabraded white patches. This gives excellent color and texture match.
- Punch minigrafting: This method is rarely used as some pebbling persists, and is reserved for areas like palms or soles where results with STG are minimal.
- Cultured melanocyte suspensions: this method involves taking a small punch of normal skin which is then sent to laboratory for melanocyte culture. The suspension of melanocyte is then spread over the vitiligo patches after superficial dermabrasion.
Laser therapy
Another innovation is therapy with an excimer laser, which produces monochromatic rays at 308 nm to treat limited, stable patches of vitiligo. This new treatment is an efficacious, safe, and well-tolerated treatment for vitiligo when limited to less than 30% of the body surface. However, therapy is expensive. Localized lesions of vitiligo are treated twice weekly for an average of 24-48 sessions.
Depigmentation therapy
If vitiligo is widespread and attempts at regimentation do not produce satisfactory results, depigmentation may be attempted in selected patients.
The long-term social and emotional consequences of depigmentation must be considered. Depigmentation should not be attempted unless the patient fully understands that the procedure generally results in permanent depigmentation. A 20% cream of monobenzylether of hydroquinone is applied twice daily for 3-12 months. Burning or itching may occur. Allergic contact dermatitis may be seen.
Skin camouflage
If the affected person is pale-skinned, the patches can be made less visible by avoiding tanning of affected skin.
Tattooing small areas of skin in mild cases, vitiligo patches can be hidden with makeup or other cosmetic camouflage solutions.
